Continue reading “Infographic: Profile of patients with PoTS (coexisting conditions)”
Category: Medical information
Infographic: Profile of patients with PoTS (quality of life)
Infographic: Profile of patients with PoTS (exercise)
Infographic: Profile of patients with PoTS (work/education)
Infographic: Profile of patients with PoTS (mobility)
Infographic: Profile of patients with PoTS (Most common symptoms)
Wheelchair “miracles”
I finally gave in and bought a wheelchair last year, when a local store had them on special.
It’s not something I need every day, thankfully. Not even most days. In fact, I’m pretty sure my Mum has borrowed it and used it for my grandmother more times than Mr Happy has used it for me! But thanks to my Dysautonomia and Ehlers-Danlos Syndrome, I suffer from debilitating fatigue, I’m unable to stand for long periods / walk long distances, and I have a propensity for dislocating body parts. So Mr Happy kept prompting that it would be handy for us own one, and after missing out on several events where I could have gone if we’d had one, I gave in.
That’s why things like this BuzzFeed post hit me really hard.
Because I know, that could have been me. Continue reading “Wheelchair “miracles””
Pacemaker Tips
I’m the kind of girl who likes to be prepared. This is probably partly because of my personality, but I think it’s also something that’s developed as I’ve grown up with a very unpredictable chronic illness. Sometimes, thinking ahead of time and being prepared can make the difference between the success or failure of an outing, trip, or event.
So that’s why, when my specialist rang me late one night and said it was time to put in a pacemaker, I found myself on Google. I was looking for pacemaker recovery tips. What did they actually do in a pacemaker surgery? What could I expect afterwards, in terms of pain, and recovery time? What kind of things could I organise ahead of time to make everything easier?
Google was very helpful in explaining what happens during a pacemaker surgery, and my surgeon was happy to answer the many questions I emailed her over the next few weeks. But I couldn’t find anything online that explained how I could prepare, what I should expect afterwards, or tips for helping with the recovery process. I turned to my chronic illness group for help, and they made helpful suggestions and answered my lingering questions.
Now that the surgery is in the past, and my pacemaker is happily ticking away, I thought I’d compile what I’ve learnt into a blog post. Hopefully, the next time someone is thrown onto the crazy pacemaker rollercoaster, they’ll find something helpful here.
Things to discuss with your doctor
What kind of pacemaker will I be getting?
Can you show me an example of the pacemaker you are planning to implant? What brand will it be? Will it have a defibrillator? How many leads will it have? Will both the pacemaker and leads be MRI safe? How long do you expect the battery will last?
How will my pacemaker be implanted?
There are two main methods of implanting a traditional pacemaker.
(1) It’s inserted under the skin (smallest impact on the body / fastest recovery)
(2) It’s inserted in a ‘muscle pocket’ that the surgeon creates by removing some muscle, or by stretching the muscle fascia over the pacemaker (harder on the body / longer recovery time – but more secure)
Surgeons usually choose the second option for people with very little ‘padding’ for the pacemaker to settle into, or with conditions that may cause the pacemaker to ‘wander’ (for example – I have stretchy skin due to Ehlers-Danlos Syndrome).
Non-traditional pacemakers, like the new, tiny Medtronic Micra are inserted through an artery in your groin. (These are not available in Australia yet, and are only suitable for some conditions).
Where will my pacemaker be placed?
Traditional pacemakers are usually put in on the left side of your chest, slightly below your collarbone, because that’s close to your heart, where the leads need to go. But it can be placed elsewhere, if there is a good reason to do so.
The non-traditional pacemakers are placed inside your heart. They don’t have leads, they attach themselves directly to the heart wall with their small metal tines.
Will you be taking any x-rays?
Having seen an x-ray of a friend’s pacemaker, I assumed that my doctor would be taking one of mine too. My husband and I were excited to see it. But when I asked for my x-rays after the surgery, the surgeon told me she doesn’t take x-rays the traditional way. Instead, she uses tiny bursts of x-ray to help her guide the pacemaker leads in. It has the advantage of being a moving picture, and is also lower in radiation. She told me that if I had asked, she could have taken an x-ray of the finished implantation for me. I was very disappointed – I had assumed x-rays of the finished product were common practice, and so hadn’t checked.
How do I care for my wound…?
For example, when you can shower / get the wound wet? Will the dressing need changing, and when? What symptoms are a warning of something being wrong (e.g. symptoms of infection, your body having an allergic reaction to the pacemaker, leads that have come out of position)? Will you have stitches that need removing, or will they be using dissolvable ones? How long after the surgery should you book follow-up appointment so your doctor can check on how the wound is healing?
How long will it be until I can…?
The elderly lady in the bed next to me had been planning to play tennis just 4 days after her pacemaker surgery! She was very disgruntled when the surgeon told her she’d need to miss the game (she kept complaining about missing out on after-game scones!) but I think the post-surgery pain convinced her.
The doctor will give you restrictions on moving your arm (mine said not to raise my left arm above my shoulder for six weeks, and not to carry anything more than 2kg with that arm for a few months). You should also refrain from doing anything involving pulling or pushing during that time – anything that’s going to stretch that area (like reaching behind yourself with your left arm and grabbing your bag from the backseat of the car). These restrictions are to prevent you from pulling the leads out of your heart – they need some time to settle in and form scar tissue around them to make them secure.
This is super easy to remember when you first get out of surgery, because the area is so painful! But once it starts healing and the pain gets less, it takes conscious effort to look after the area. (Reader tip: If you keep waking up and finding yourself with your left arm stretched above your head – wear a bigger shirt, and sleep with your left arm tucked inside it, down by your side!).
Check with your doctor when you can resume the specific activities you like to do (e.g. driving, playing tennis). I had to check when I could fly, so that I could return home after the surgery (my surgeon suggested a minimum of one week post-surgery).
Once I have a pacemaker, will I still be able to…?
After you recover from surgery, you can resume most activities as normal. But there is a list of things that you can’t do (or it’s strongly suggested that you don’t do) when you have a pacemaker. Most of these involve some kind of machinery that may interfere with the working of your pacemaker (e.g. welding equipment), or an environment that puts too much stress on your heart (e.g. scuba diving).
Medtronic has a list of devices sorted into three risk categories: no known risk, minimal risk, and special considerations here. It also includes a list of dental and medical procedures you can or can’t have once your pacemaker is implanted. If there’s anything on the red list you want to do / use, make sure you discuss this with your doctor before getting a pacemaker inserted.
Other questions to ask:
Do I need to stop taking any of my medications before the surgery?
Where will the surgery take place?
Who will be doing the surgery?
Who will be my anaesthetist?
How much will it cost?
Do you / the anaesthetist have a no gap policy?
(In Australia, this means that they won’t charge you anything extra on top of what insurance will pay them. If you have private health insurance, check to see what parts of your surgery / fees / hospital stay they will or won’t cover. Mine covered everything – I just had to pay a set excess fee to make the claim.
How long will I stay in hospital after the surgery?
(I just stayed in overnight – but the length of your stay will depend on your
health conditions / your age / the kind of surgery you’re having done, surgical complications etc)
Things to pack
- Button up shirts
After the surgery, your shoulder will be stiff and your chest will be very sore. As well as the pain and swelling restricting movement, you have to be careful how you move your arm while the leads are still settling in. This means that normal T-shirts aredifficultpretty much impossible to get into. Packing button up shirts was the best tip someone gave me before surgery. It made getting dressed and undressed much easier.
- Strapless bras / ‘genie’ bras
Most women assume they won’t want to wear bras for a while after their surgery. This really depends on the size of your “verandah” though. Whenever you are upright, gravity will make your bra-less verandah sag a bit, pulling painfully on the incision in your chest. Lying down in bed (which you’ll probably be doing a lot of) it’s generally more comfortable to go bra-less, but it’s good to have the option of a bra if you are going to be wheeled down the corridor for testing, or to go to the toilet.I found strapless bras were the most helpful to start with, and then soft genie bras in a size or two above what I’d usually wear in the weeks afterwards (I didn’t put the strap of these over my left shoulder, but instead tucked it into the side of the bra, and just had the one strap over my right shoulder holding it up).
- Headphones + audiobooks and device pre-loaded with movies
I had a looooooong, mostly sleepless, first night after my pacemaker was implanted. I had taken my Kindle, but found I wasn’t up to reading a book (it didn’t distract me enough from the pain). Thankfully I had also packed a pair of good headphones and some devices pre-loaded with audiobooks and TV shows. This meant I could spend the night listening to Stephen Fry narrating Harry Potter, alternating with watching episodes of Merlin on a borrowed Samsung tablet (thank you Tina! That was a lifesaver!!!)
Oh – and don’t forget to pack chargers for all your devices!
- A printed list of your allergies and reactions + medications
I have quite a few allergies and intolerances, and this list saved me so much time and brainpower. I take it with me whenever I go to hospital. Make sure the list states both the thing you are allergic/intolerant to and also what happens when you take it / why you can’t have it. If you’re on a few medications, take a list of those too. And always take all your medications with you when you go to hospital – you’ll probably need to keep taking them (but of course, check with your doctor!).
- Food / water
I am very limited in what I can eat, and I can only drink a certain brand of water – anything else makes me violently ill. So my husband organised with the nurses to keep my special food in a little fridge close to my room, and he would pop by at meal times to feed me. We put the water next to my bed where I could reach it, and I was set.
- Toilet paper
This might seem like an odd one, but it came in handy! You’re confined to your bed for a while after surgery (you can read about what happened when I tried to ignore that rule here…). This means your toileting options are (a) bedpan while lying in bed, or (b) bedpan on a chair next to your bed because the nurses take pity on you when your body absolutely refuses to wee while you’re lying down. Having a roll of my own toilet paper right there meant I didn’t have to wait for the nurses to bring me some, and I could skip the embarrassment of buzzing the nurses to ask for more than the three tiny, translucent squares they’d given me. It also meant I didn’t have to worry about allergic reactions. Yes – you can be allergic to toilet paper! Or at least, to the perfumes and fragrances they’ve spritzed it with, or the ink they used to print that seashell design. Seriously – I’ve just had surgery. The last thing I need right now is an allergic reaction down there. So I’ll just use my own, thanks!
The roll also came in handy for non-toileting uses, like cleaning my iPhone screen, wiping up the cereal I’d just spilled down my front while trying to awkwardly eat around a sling / blood pressure cuff / pulse oximeter / IV tube, and stemming the flow of saline and blood shooting out from the cannula when the IV malfunctioned…
Things I wish I’d known beforehand
Pacing sensation
Your pacemaker data is easily accessible, and the settings are easily changed. They just place a device that looks like a large computer mouse on top of your chest, and your pacemaker talks to it. The large computer mouse looking thing talks to a computer, and they make adjustments on the computer. The process is completely painless and non-invasive.
BUT…I can feel when my pacemaker kicks in and starts controlling my heart rate. It’s hard to describe – but it’s a very odd sensation. The closest I can describe it is that it feels like the butterflies you get in your stomach – but in your heart! It’s not painful at all, it just feels…strange! Especially when the pacemaker technician comes and tests different settings with that large computer mouse thing. The good news is you do get used to the feeling. It was just something I was unprepared for – and I feel like knowing beforehand might have been helpful.
Pain and the healing process
Several friends who already had pacemakers inserted warned me that I should expect lots of pain post-surgery (particularly since I was having the more-intense implantation done, involving the muscle). My friends also told me to be sure to let the nurses know when I was in pain, because it’s easier to get on top of the pain when, for example, you’re at a 6/10 level of pain, than it is when you’ve reached 10/10.
So once the medications they had used in surgery and the recovery ward wore off, I asked for pain relief. Unfortunately, the medication the nurses on the general ward gave me did absolutely nothing to relieve my pain. That wasn’t their fault; they gave me a strong medication. But it seems that my body didn’t know how to use it. Once they’d given me that, the only other thing they could offer me was Panadol (which, sadly, also did nothing for my 10/10 pain).
I was very thankful for my friends’ warnings. At least I went in mentally prepared, and wasn’t surprised by the long, sleepless night that followed the surgery. What I was surprised by was how long that high level of pain lasted. I spent the week following the surgery in a state of 9/10 pain. The nurses had offered me a script of strong pain killers when I was released from hospital, but since it was the same medication I’d tried several times that night with no effect, it seemed a bit pointless, so I declined it. If I’d known ahead of time that I was going to be in that much pain, for that long, I definitely would have organised different, better pain relief! (The nurses couldn’t offer me anything different, but I could have insisted on speaking to my doctor about an alternative). The medication they gave me in hospital is going to get added to my list of allergies and reactions, with a notation next to it saying, “This medication has no effect – don’t bother giving it to me!”
Pre-surgery, whenever I thought about the healing process, I mostly just thought about the incision site. How long would it take for the incision to close? What would it look like afterwards? I gave a thought or two to the poor muscle that was going to be abused to fit the pacemaker in there, but mostly I just thought about the cut they were going to be making.
I had no idea that after I’d healed from the surgery, there would still be pain and / or discomfort. Don’t get me wrong – I think my pacemaker is wonderful, and I’d still choose to have it put in. But I didn’t realise it would be so… uncomfortable, even after the wound had ‘healed’. I don’t know why I thought having a metal thing smooshing around inside my chest could be comfortable: it seems pretty silly now. But it just never occurred to me. I’m now five months post-surgery, and I still have to be careful how I lie on my stomach (which is how I sleep) – if I press too much on the pacemaker site, it hurts. If Mr Happy gives me a hug, we have to angle ourselves a certain way so that my left shoulder/chest doesn’t get too squished, because that hurts. I don’t bend down to hug small children anymore, because during their enthusiastic, wiggly hugging, my pacemaker site will inevitably get bashed with an elbow or bony chin, and that hurts.
Apart from pain, there’s the itchiness. There’s no redness or hotness – it’s not infected. The incision scar and skin over the pacemaker is just itchy, probably as part of the healing process. But it’s not very nice, because there’s no way you can scratch it – the skin is too tender, it feels like scratching a burn. Icepacks help take the itchiness away – any creams I’ve tried have just made the itch worse.
Here’s my scar: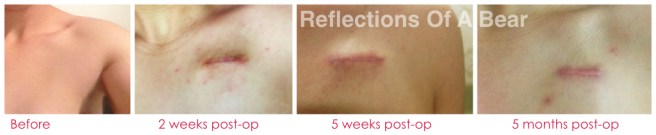
I’ll finish with some bathroom selfies, because… why not? My scar doesn’t embarrass me, not one tiny bit. Why should I be self conscious about a mark left from an important medical procedure? 
I’m just thankful to have my pacemaker ❤
It hasn’t improved my blood pressure or fatigue, but it’s made a world of difference to my syncope episodes. Now, instead of my heart rate bouncing up and down and up and down, and eventually stopping, my pacemaker kicks in. So instead of passing out, and then spending the next few days pale and shaky, I can lie down, and twenty minutes later, I’m feeling back to normal.
That was a long post! I hope someone, someday finds it helpful.
xx S.
NB: The wonderful Rachel from The Chronicles of Rach pointed out a checklist with all this info would be oh so handy, as then you could actually take it with you to the doctors appointment! She’s right, so here it is! >>> Pacemaker Checklist. It’s totally free for you to use ❤
* * * * *
Update: January 2017
I had my pacemaker implanted in June 2015. In the first five months alone, it saved my heart rate from bottoming out 645 times! Unfortunately, an x-ray at a checkup in late November 2015 showed one of the leads of my pacemaker had come out of my heart wall, and was just dangling in my heart. So I had to have surgery a second time in Dec 2015, to have the leads repositioned. It’s been working fantastically since (I very rarely pass out now) and I’ve not had any problems with the leads again.
Heartache
White halls.
White doors.
White walls.
White floors.
“That rhymes,” I tell myself.
Anything to stop me from thinking about where I am. Continue reading “Heartache”
Captain of your health (part 2)
This is the second of two posts about navigating the medical system.
If you haven’t read part 1, you can find it here: Captain of your health (part 1) Otherwise, read on!
During appointments
Phew! You got an appointment! After all that effort, the last thing you want to do now is waste it. So how do you get the most out of an appointment?
Continue reading “Captain of your health (part 2)”
